“Don’t let the ‘me’ intervene, my father always cautioned me,” says Dr. Abdul Bari. And that piece of wisdom is something he has lived by. The founder and CEO of the Indus Hospital and Health Network — the largest free of cost medical service in Pakistan — Dr. Bari remains remarkably approachable and free of any sense of self-importance. Bearded and bespectacled, any gravitas is belied by his ready smile and open, courteous demeanour.
Starting operations in 2007, the Indus health network has grown from a single hospital in Karachi to a health network spread across Pakistan. It encompasses 13 hospitals, eight of which are government hospitals being run as public-private partnerships. There are four blood centres and four rehabilitation and artificial limb centres. Their primary health and outreach programmes touch 51 districts, including a boat clinic, and an increased focus on telemedicine. And many more projects are in the pipeline.
Dr. Bari’s family hails from Peshawar but he was raised and educated in Karachi. “My father moved to Karachi in 1956,” he says. “I am a true Karachiite.” After graduating from Adamjee Science College, he studied medicine at Dow University (Medical College at that time) and later did his post-graduation in Cardiac Surgery from Karachi as well.

“I come from a middle-class background. We are a family of 11 siblings and we grew up in a small apartment. My father was a very religious man and he had a particular habit. After his prayers, he would always pray aloud. And for me, he always had one prayer, ‘Ya Allah, make Bari serve humanity in his career as a doctor.”’
Studying at Dow Medical College and the affiliate government-run Civil Hospital, the young Abdul Bari and others like him were acutely aware of the problems faced by patients. Some years earlier, a few students had formed the Patients Welfare Association with an aim to provide some relief.
“I joined the Association in 1980,” recalls Dr. Bari. “There was a cupboard in the office of our professor, Surgeon Mushtaq and that was our treasury. We would collect money and buy medicines to give away.”
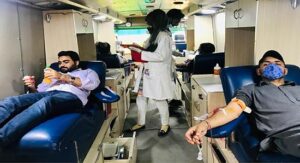
Unbelievable as it seems now, till the eighties, blood banks were completely dependent on professional donors. “Here was a permanent line of professional donors outside Civil Hospital,” explains Dr. Bari. “They had a thekadar called Kalay Khan. He would yell out the blood group needed and the donors would line up.”
A healthy individual can donate blood once in three months but these donors were giving blood every week. “They would take saline drips in between, so their blood was not only diluted, low in haemoglobin, but also infected with hepatitis, malaria, and you name it…”
Then in 1981, the professional donors went on strike to lobby for higher remuneration. This proved to be the impetus needed to change the system.
Dr. Bari was a second-year student at the time. “There was no other source of blood and we realised that we could not be hostage to these people,” he says. “We needed to set up our own blood bank with voluntary donors.”
Dr. Bari was made the director of this project and he and his band of colleagues set to work. They were allotted a room which had to be repaired and re-constructed. “We would work late into the night supervising things. And we were also going up against a mafia so there was a level of stress. We would always go home in groups when it got late.”
Then there was the task of motivating people to give blood and collecting rare blood groups etc. Initially, medical students were the best scouting ground for blood donors. “We were known as the vampires,” laughs Dr. Bari. But the biggest challenge was changing mindsets and eradicating erroneous beliefs about donating blood. “I remember arguing with a man whose wife urgently needed blood. I told him she will die if you don’t give her blood. But his logic was that if he did so, she would become his sister. The family was actually willing to let her die.”

Slowly the message was heard and it spread. “The system changed, volunteerism prevailed and now professional donors have vanished. It took time, 30 years, but that is how long real change takes.”
The blood bank had been set up but patients were given whole blood which was a tremendous waste.
Dr. Bari floated the idea of setting up a blood fractionation system to the Patients Welfare Association. A fourth-year student at that time, he and his colleagues were on study leave. “We got machines and training from Germany and I learnt to separate blood into plasma, platelets etc.” This training was then passed on to the technicians at home. The most intimidating part for Dr. Bari was telling experienced doctors to change the way they were working. “My mentor Surgeon Mushtaq told me to prepare a presentation on the subject which he would allow me to present at a surgeon’s conference to be held in Karachi. He helped me practice, I would go to his house and he would time me.” Thanks to those efforts, today, it is common practice in Pakistan to separate blood into its various components and administer only what is needed.
All these experiences with the Patients Welfare Association groomed Dr. Bari for the task he would take up in future. “I learned motivation, procurement, and how to deal with donors.”
From the beginning, the association had one inviolable code: there would be no personal projection of any individual. “I recall I was invited to a show on PTV to talk about the work done with the blood bank. There was a lot of debate within our group and finally they decided I shouldn’t go. The producer was very surprised.”
The eighties were a turbulent time in Karachi. In 1986, a massive bomb blast in one of the city’s oldest and busiest markets, Bohri Bazaar, shook the local community. “I was doing my house job then and I clearly recall the carnage. Picking out survivors from the bodies which came in… At that time, I saw how the city responded to the tragedy. People were lining-up to donate blood, waiting with bags of money to give.” This assured Dr. Bari of the immense potential for charity and the work it could support.
The Patient Welfare Association decided to upgrade the over-burdened Emergency Ward at Civil Hospital. A committee was formed and the architecture firm of Arshad Shahid Abdullah volunteered their design services. The project was budgeted at 36 lakhs and fund raising began. “We launched a programme targeting schools. We would go and give presentations and plastic money boxes were left at the schools to collect money.” Out of the 36 lakhs needed, 24 lakhs were raised from the school campaign. “About 3 lakhs of this was received in coins stuffed into 40 sacks.”
The night before the inauguration of the new Emergency Ward, Dr. Bari was with the project team of doctors, architects and planners. “And I said to them ‘If God wills it, one day we will build a hospital which provides quality care free of cost.’ And so the dream was born in 1987.”
Later that year, Dr. Bari’s colleagues and friends went abroad for their post graduate studies. Dr. Bari’s father was a paraplegic at this time and he did not want to leave the country. So he remained in Karachi and trained at the NICVD as a cardiac surgeon. “Surgeon Rahman was my mentor there,” recalls Dr. Bari. “The institute provided quality care but was very limited with only ten beds and two theatres. The waiting list stretched three years during which most patients didn’t survive.”
By this time, the young Dr. Bari knew a thing or two about fundraising and project building. “I had some credibility by now and enjoyed donor confidence.” He took on the task of expanding the Cardiac Unit at NICVD. “Tariq Qaiser who had designed our Emergency Department building, as a young architect with Arshad Shahid Abdullah, had his own firm now. He designed the new space for us, we raised funds and began construction within three months.” The new unit was attached to the old one and it was a challenge cordoning off areas and carrying out construction while the rest of the hospital continued to function.
Meanwhile, another important event in Dr. Bari’s life was coming up. ‘I had to fly to Peshawar for my wedding,’ he says. “The rest of my family had already left. We had a shortfall of 5 lakh rupees for the NICVD project and I was very worried about it. I was in contact with someone about a potential sponsor but it was very uncertain. That night I went to sleep and suddenly woke up in cold sweat. I kept tossing and turning and couldn’t sleep. Then I got up and said my prayers. ‘Oh Lord, when I leave the city tomorrow may it be without any burden on my shoulders.’ After that I slept peacefully.” The next morning when he went to work, he got a call from a donor, who pledged the remaining amount.
In 1995, Dr. Bari did his fellowship to become an Assistant Professor of Cardiac Surgery. It now became his mission to establish a Department of Cardiac Surgery at Civil Hospital where none previously existed. Dr. Bari formed the Friends of Cardiac Surgery and set about raising funds for the task. “I went back to the same donor who had funded the last five lakhs for the Emergency Ward. He agreed to give me the money on the condition that I take his son under my wing and allow him to assist me on the project.”
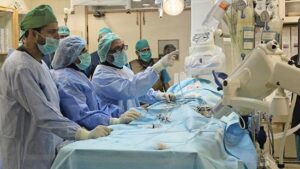
In 2000, the first cardiac surgery was performed in Civil Hospital by Dr. Bari’s mentor Surgeon Rahman. After that, a flood of patients followed. Dr. Bari continued working at Civil Hospital till 2018 when he took early retirement.

But during his stint at Civil Hospital, he had not forgotten his most ambitious dream of building a free hospital. In 2004, Dr. Bari’s doctor friends returned from abroad. “I reminded them of our dream and said that the time had come to realise it.” They set up a foundation with some 17, 18 people on board and started scouting for land. Then someone told them about the Islamic Mission Hospital and Nursing School which had been set up with funding from Abu Dhabi. “But the project had run into financial issues and couldn’t get off the ground. The building was already there and so, we decided to take over that project.”
In 2005, Pakistan was devastated by an earthquake and Dr. Bari and his team left for northern Pakistan where they ran a field hospital in Balakot.
In 2007, the focus shifted back to Karachi and the Indus Hospital started operations with 150 beds. “We had no money but we had faith and determination,” says Dr. Bari. “Everyone was skeptical of the model of a free private hospital. They all said it wouldn’t work.”

So why didn’t the team opt for a model which combined donations and profit from the affording? “Because I have seen that model fail,” insists Dr. Bari. “After one generation it becomes a profit-based private hospital. And there is no way that all patients will be treated equally. There will be a difference between those who pay and those who don’t.” Dr. Bari also holds another ideal in mind. “Historically, in any Islamic society, three things were the responsibility of the state: health, education, and inns for travellers.”
His belief and determination prevailed. Today, 15 years on, the Indus Hospital network is firmly established and growing. Their annual budget has grown from millions to billions of rupees and sees an increase every year.

While Dr. Bari was chasing his goals, his wife, also a doctor, remained his pillar of support, holding up the home front. “I had told my wife of my mission while we were still engaged, and she always encouraged me. I saw my children grow up horizontally,” he laughs, referring to the fact that they were mostly sleeping when he got home. “But one thing I did was to always drop them to school in the morning — from school right up to university.”
When the couple’s three children, two boys and a girl, were a little older, Dr. Bari’s wife did a post-graduation in family medicine but later took a degree in hospital administration. Today, she is part of the Indus Health network. “So our missions aligned,” he smiles. “With the advantage that we are both so tired when we come home, there are no fights,” he jokes.
What has been the biggest challenge in pursuing his dream? ‘Money has never been the problem,’ says Dr. Bari. “Once you have people’s trust, you will find they are looking for good ways to spend their money. The biggest challenge has been that of human resources.” What is Dr. Bari’s future vision for the Indus Network? “Health is not only physical and mental, it is social and environmental,” he maintains. “Only if people are lifted out of poverty can there be a true cure. We must adopt a holistic, multi-sectoral approach towards a larger goal. We need to connect with like-minded people so we can see an impact.”
Dr. Bari would like to see the Indus network become a bridge to connect different sectors like education, agriculture, health etc. “We have to focus on all the creatures of God. This includes the veterinarian sector and we have also started a rabies vaccination programme for dogs.”
Dr. Bari believes that public-private partnership is the way forward. “We must put ourselves in a position where we can influence policy making. Everyone has their strengths. No one can get results alone. Nor us, nor the government. But if we all work together, it’s a win-win. And this has been seen in the handling of the COVID-19 crisis.” Although Dr. Bari’s father did not live to see the Indus Hospital, he knew that his son was on the right path. “I can’t become complacent about it. One has to do jihad with oneself every day.”
The writer is a prominent freelance journalist and runs her own interiors and lifestyle online publication.

